Retinal Detachment: A Practical, Patient-Centered Guide to Saving Vision in Delhi
- Updates
- 1 day ago
- 3 min read
If you ever see flashes, floaters, or a dark curtain in your vision, please come in right away. It could be something serious, like retinal detachment.
Let's talk about retinal detachment in a way that is easy to understand, honest, and clinically useful in Delhi.
What does it mean to have Retinal Detachment?
The retina is thin, light-sensitive that is inside your eye. It works like a camera sensor by taking pictures and sending signals to the brain.
This layer separates from the back wall of the eye, cutting off its blood supply, which causes retinal detachment. It can cause permanent loss if vision if not treated right away.
What Causes Retinal Detachment?
Let's break it down into causes that you might be able to relate to:
1. Age-Related Changes
As we age, the gel inside the eye (vitreous) shrinks and pulls on the retina. This can create a tear.
2. High Spectacle Power (Myopia)
People with high minus power have thinner retinas, making them more prone.
3. Eye Injury
Even a blunt injury can trigger detachment.
4. Previous Eye Surgery
Especially after cataract surgery in some cases.
5. Diabetic Eye Disease
Uncontrolled diabetes can cause tractional detachment.
6. Family History
Genetics can play a role.
What Does a Patient Actually Feel?
This is important—because early recognition can save vision.
Patients often describe:
Sudden increase in floaters (black dots, cobwebs)
Flashes of light, especially in dim light
A shadow or curtain moving across vision
Blurred or distorted vision
Important point:
People often wait to come in because retinal detachment doesn't hurt.
How do we figure out what it is?
The method is systematic at places like Claritas Eye and Retina Institute.
A Detailed History
Exam of the Dilated Retina
Optical Coherence Tomography (oct)
B-Scan Ultrasound: used when the retina isn't clear (for example, when there is bleeding)

Step-by-step approach to treatment
Let's make this easier:
Step 1: Figure out what kind
There are three main types:
Rhegmatogenous (tear-related)- the most common type
Tractional- most of the time, it's from diabetes
Exudative means that there is inflammation or fluid
Treatment Choices (And When We Use Them)
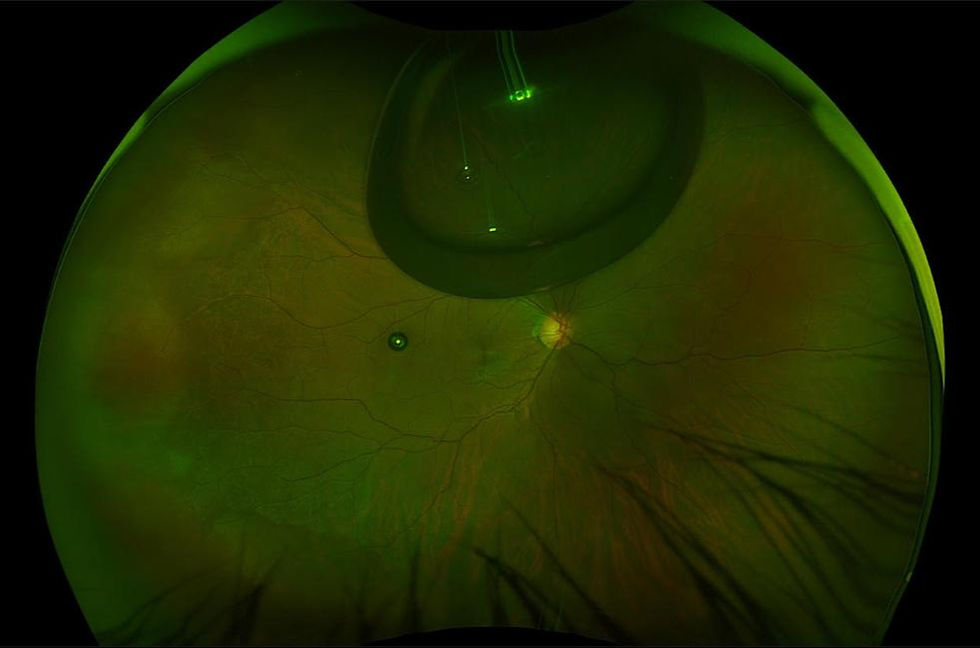
1. Laser Treatment (Retinal Tear Only)
If caught before detachment:
Laser seals the tear
Prevents progression
Best for early-stage cases
2. Pneumatic Retinopexy (Gas Injection)
A gas bubble is injected into the eye
Patient maintains a specific head position
The retina reattaches as the bubble pushes it back
Best for:
Small, superior detachments
Selected cases


3. Scleral Buckling Surgery
A silicone band is placed around the eye
Relieves traction on the retina
Best for:
Younger patients
Specific tear configurations
4. Vitrectomy Surgery (Most Common Today)
This is the most advanced and widely used technique.
Vitreous gel is removed
Retina is repositioned
Laser is applied
Gas or silicone oil is inserted
Best for:
Complex detachments
Diabetic tractional cases
Large or multiple tears
Which Treatment is Most Efficient?
There’s no “one-size-fits-all.” The best option depends on:
Condition | Best Treatment |
Small tear, no detachment | Laser |
Early, simple detachment | Gas injection |
Peripheral detachment in young patients | Scleral buckle |
Complex / diabetic / large detachment | Vitrectomy |

What Happens If You Delay Treatment?
Let’s be very clear here:
The longer the retina stays detached, the lower the chance of visual recovery
If the macula (center of vision) is involved, vision loss may be permanent
This is why we treat it as an emergency
Recovery: What Patients Should Expect
Vision recovery may take weeks to months
Positioning may be required (especially after gas injection)
Avoid air travel if gas is inside the eye
Regular follow-ups are essential
FAQs (Real Questions Patients Ask)
1. Is retinal detachment painful?
No, it is usually painless—but visually disturbing.
2. Can it heal on its own?
No. It always requires medical or surgical treatment.
3. Will I regain full vision?
Depends on how early it is treated and whether the macula is involved.
4. Is surgery risky?
Modern retinal surgeries are highly advanced and safe, but like any surgery, they carry some risks.
5. Can it happen again?
Yes, especially in high-risk individuals. Regular check-ups are important.
6. How urgent is it?
It is an emergency. Same-day or next-day consultation is ideal.
Final Thought
If you ever notice sudden floaters, flashes, or a shadow in your vision—don’t wait, go ahead with your dilated retina examination.
At Claritas Eye and Retina Institute, under the guidance of Dr. Mayank Bansal, the focus is always on early detection, precise diagnosis, and customized treatment—because in retinal detachment, time is vision.




Comments